When it comes to bedsores and dementia, it is important to know how to approach with treatment, or even better, have a prevention plan in place.
Bedsores can develop quickly – in as little as a few hours. It’s best to prevent them if possible. If they do develop, it is vital they are tended to promptly.
Prevention & Treatment for Bedsores and Dementia
They can be extremely challenging to treat and can be quite detrimental to a person’s health and quality of life.
What are Bedsores?
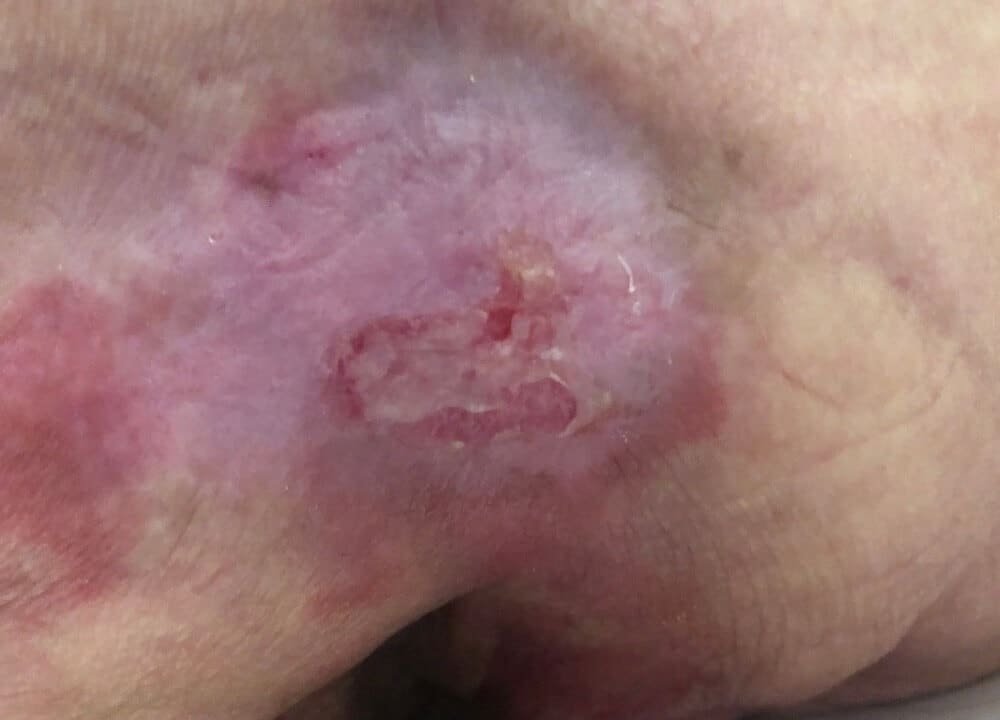
Bedsores are also known as decubitus ulcers, pressure sores, pressure ulcers, or pressure injuries. They develop when an area of skin and underlying tissue loses blood flow and starts to die.
This can occur when a shoe, medical device, or other object presses against the skin over an extended period of time.
One of the most common causes of pressure injuries is when skin and tissue are compressed for a sustained period between a person’s skeleton and a surface such as a mattress or a chair.
People who are able to move and reposition normally will adjust their weight frequently enough that blood remains flowing and skin remains healthy.
People who aren’t able to reposition themselves easily, and who spend a lot of time sitting or lying down, are at the greatest risk for developing a pressure ulcer.
Why are Pressure Ulcers a Problem?
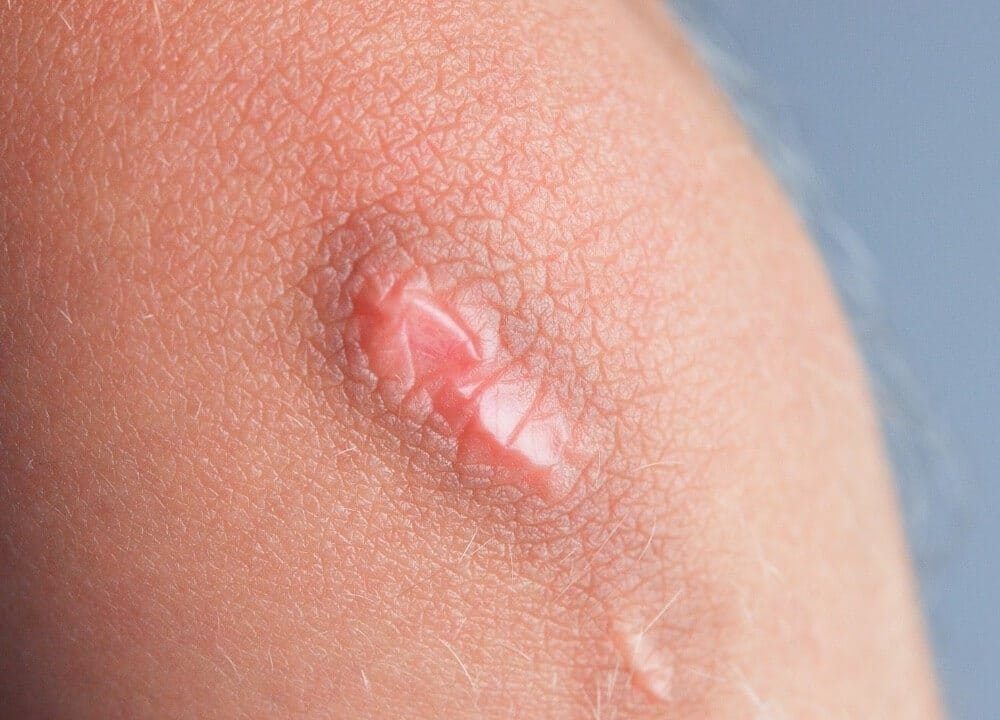
While pressure ulcers often develop quickly, they can take an extremely long time to heal.
Factors that contribute to their development – such as limited circulation, impaired mobility, poor nutrition or compromised health – often work against their healing.
Pressure sores are associated with many complications, especially infections.
They often take a great deal of bodily energy to heal – energy which people in poor health usually lack.
Pressure ulcers can be very uncomfortable or painful, detract from quality of life, and in some cases, they can contribute to an earlier demise.
Suggested Products to Assist People with Bedsores and Ulcers
[table id=19 /]
A Particular Challenge in People with Dementia

People with dementia may have difficulty moving their bodies.
Even if they are painful, they may not recognize that moving would relieve the pressure and pain.
They may not understand the need to reposition themselves to prevent a pressure injury, and may not be compliant with caregivers’ attempts to do so.
For example, a person may prefer to sleep on his or her back all night. He or she may resist lying on the side, or may scoot back to their back shortly after moving off it.
Once a pressure ulcer develops, someone with dementia may not be compliant with the measures needed to heal it.
Aside from keeping pressure off the affected area, bedsores often require painful wound care.
People with dementia may react with uncooperative or resistant behaviors, including pushing, hitting or kicking at caregivers.
In many cases, people with pressure injuries are repositioned every two hours around the clock. Being awakened frequently can cause sleep deprivation and an array of physical and emotional effects for people with dementia, including:
- Uncooperative or difficult behaviors
- Daytime sleepiness
- Withdrawal from social interaction or activities of interest
- Decreased physical strength and coordination
- Decrease in cognitive function
- Increase in emotional volatility
- Changes in eating, appetite, nutritional status and weight
Four Stages of Pressure Sores
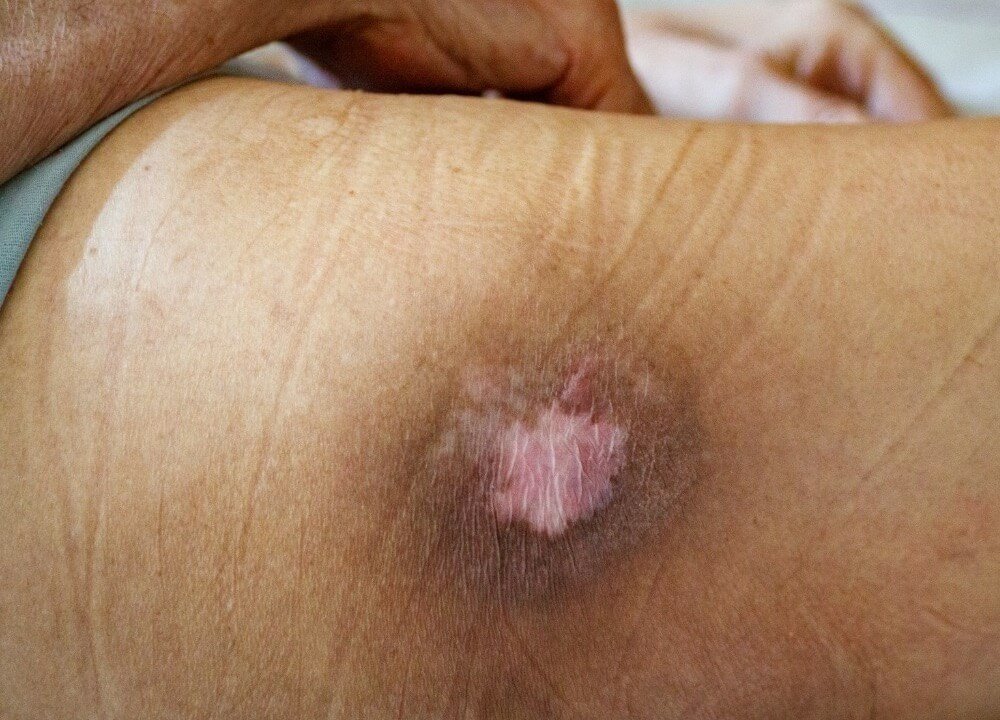
Pressure ulcers are categorized into four stages based on their severity.
Stage 1
Stage 1 pressure injuries are the first, and mildest, stage. The skin is not yet broken, but it usually looks discolored – usually reddened in light skin, and slightly purple or blue in darker skin. (Dark purple or maroon usually indicates a deeper injury.)
When pressed with a finger the area does not turn white.
A stage 1 bedsore may be warmer, cooler, firmer or softer than surrounding skin. It may or may not be tender or painful.
Stage 1 pressure ulcers are the easiest to heal, but they will progress into stage 2 quickly if the pressure is not relieved.
Consult with the person’s doctor if they don’t resolve within 24-48 hours after relieving pressure.
Stage 2
Stage 2 pressure injuries feature broken skin with pink or red moist wound beds. Blisters may be present, but no underlying tissue is involved.
Stage 3
In stage 3 pressure injuries the tissue beneath the skin is visible. Stage 3 pressure injuries can be very extensive beneath what is immediately visible.
Stage 4
In stage 4 pressure ulcers muscles, tendons or bones may be visible. Black, dead tissue may be present.
Stage 3 and 4 pressure injuries are serious medical issues and require the support and guidance of a medical team to help them heal.
You should consult the individual’s doctor for all pressure injuries. Even Stage 1 pressure injuries should be viewed as a warning taken very seriously.
The doctor should take measures promptly to ensure they don’t worsen or recur.
Sepsis: A Medical Emergency
Pressure ulcers can easily become infected, especially if they are exposed to bacteria from stool or other bodily fluids.
Signs of an infected pressure sore may include:
- Redness, soreness or heat in the skin around the pressure injury
- Pus or drainage from the wound
- Foul odor from the wound
- Fever
When you notice signs of infection, notify the person’s doctor promptly.
Because it is easy to miss signs of infection, it’s important to be alert for signs of sepsis in people with pressure ulcers, even if there isn’t a known infection.
Sepsis is a severe reaction to an infection in which the body’s organs shut down.
Without emergency medical treatment, it can rapidly lead to death. Get the person to the emergency room right away and tell them you suspect sepsis.
Look for:
- Signs of infection
- Temperature changes (high fever or abnormally low body temperature)
- Mental changes (increased confusion, extreme sleepiness)
- Signs of extreme illness (shortness of breath, discomfort, weakness, pain)
What Contributes to Bedsores?
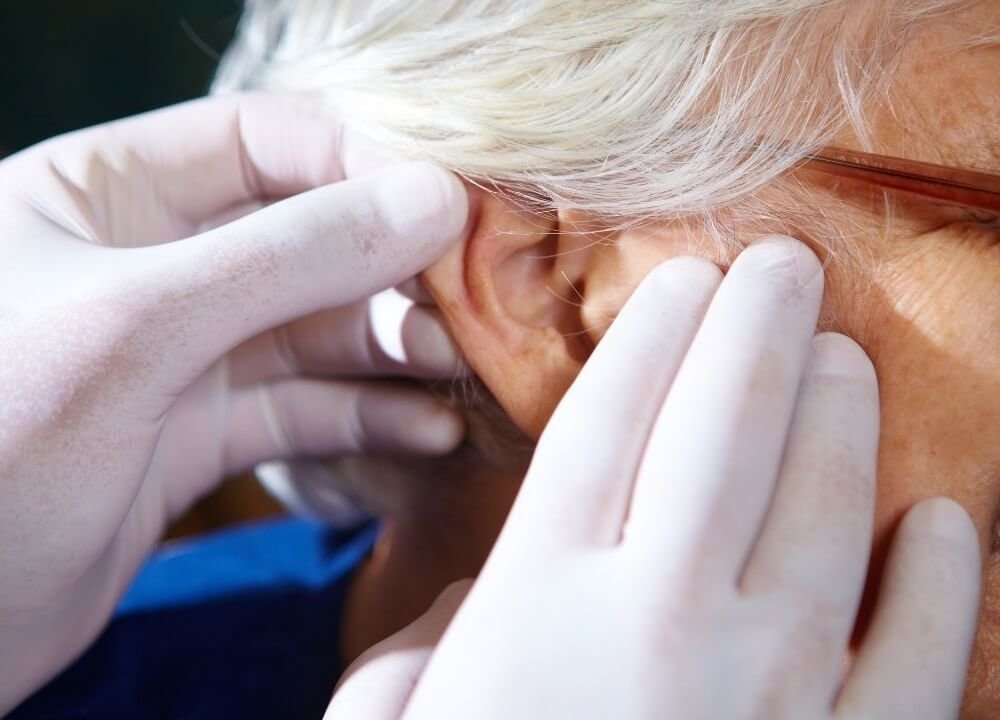
Pressure sores are especially common in areas over bony prominences that experience sustained contact with a chair or bed.
Areas that are particularly prone include:
- Ears
- Shoulder blades
- Spine
- Tailbone
- Elbows
- Hips
- Knees
- Ankles
- Heels
Sustained pressure
Pressure ulcers can start to develop within a mere two hours when the pressure between the person’s bone and a chair, bed or object has cut off blood flow to the skin and underlying tissue.
Friction
Friction occurs when skin rubs against another surface, such as when a person is pulled up in bed by caregivers.
Shear
Shear occurs when skin stays in one place while bones move. This pinches off blood vessels and restricts blood flow. A common example of shear is when the head of a bed is elevated and a person slowly slides downward.
Poor nutritional status
Dehydration, unplanned weight loss and general malnutrition are known to be significant risk factors for developing pressure ulcers.
Incontinence or wetness
Urine and feces are especially caustic to the skin. Moisture from incontinence, perspiration or other sources can weaken the skin and make it more susceptible to damage.
Immobility
When someone spends a great deal of time in bed or in a chair and doesn’t move or reposition themselves frequently, they are at high risk for developing pressure ulcers.
Can Bedsores Heal?
Bedsores can heal, but it is far easier to prevent one than it is to heal one. Catching and treating it as early as possible makes a huge difference.
Compliance with keeping all pressure off the affected area is extremely important – and often, extremely challenging. It may be necessary to alter one’s sleeping or sitting position for an extended period.
Usually, the pressure ulcer develops in the first place because the person favors that position for some reason. (Such as someone who sleeps on their back due to breathing or discomfort may need to adapt to sleeping on their sides instead).
Refraining from it can be uncomfortable, inconvenient, or present other challenges.
How to Prevent Bedsores

Repositioning
Most people without mobility impairments reposition themselves frequently when sitting or lying.
If someone doesn’t reliably reposition themselves independently, a caregiver should remind and assist him/her to do so.
Many facilities use every two hours as a standard for repositioning, however, the need will vary by individual. Also, there is rising concern about the detrimental effects of sleep deprivation when people are repositioned this often.
The person’s doctor or medical team should determine the frequency of repositioning based on their unique situation.
Repositioning doesn’t necessarily need to be a significant amount of movement.
A shift in weight or a slight turn to one’s side may be sufficient as long as it relieves pressure.
Use pillows under arms or legs, between knees, or behind backs to support their body as needed.
Minimize Friction and Shear
Keep the head of the bed elevated only as much as needed, and elevate the feet to reduce sliding and minimize shear.
When pulling someone up in a bed, lift them fully off the bed, rather than letting them drag against the sheets.
Special friction-reducing sheets designed for this purpose may be helpful.
Nutrition
Wound healing benefits from extra calories, protein, zinc, certain vitamins and amino acids.
Hydration is an extremely important factor in both preventing and healing pressure ulcers.
Different people have different nutritional needs.
For example, people with kidney impairment may need to avoid too much protein or limit fluids. Consult with a doctor or dietician regarding an individual’s nutritional plan.
Keep Skin Clean and Dry
Remaining in a wet or soiled brief is extremely hard on the skin. Ensure to promptly clean all incontinence episodes.
For frequent incontinence, use a barrier cream to protect the skin.
Incontinence products designed for overnight use can help. Such products aim to hold urine away from the skin so it stays dry.
These products tend to be more expensive, but worth the extra cost in some cases.
Minimize episodes of incontinence by following a person-centered toileting schedule when possible.
Mobility
Encourage and assist an individual with dementia to retain their mobility to the extent possible.
When safe and practical:
- Move the person out of a wheelchair into a dining chair to eat
- Get up to the toilet, move about or switch seats every two hours
- While it can feel natural to essentially wait on someone who has difficulty getting up, look for opportunities to allow them to get up and do for themselves. What we don’t use, we lose!
Consult with a doctor, physical therapist or personal trainer regarding ways to keep the individual mobile.
Be sure to find a physical therapist or trainer who has the experience and is comfortable working with dementia.
Because people with dementia may not remember their instructions, it takes a particular skill set to achieve the best benefit.
Finding the right therapist or trainer can make all the difference in the person’s success.
Routine Skin Checks
Make a habit to visually inspect the person’s skin routinely. Pay special attention to their bony prominences including toes, ankles, heels, knees, hips, tailbone, spine, shoulder blades and ears.
The recommended frequency of routine checks will vary based on the individual and their unique health status. Check with their doctor for specific recommendations.
Generally, it’s a good idea to inspect all areas of skin at least daily for high-risk persons.
The coccyx should be inspected with each brief change when incontinence and limited mobility are concerns.
Diabetic Feet
Pay extra attention to the feet of someone with diabetes. The impaired circulation to these lower extremities exacerbates the risk terribly.
Socks and shoes should always be clean, dry and fit properly.
Specialty cushions or equipment
Pressure reduction products, such as cushions and other equipment, are available to help reduce the risk of bedsores.
There are many factors that contribute to pressure injuries, and they vary considerably by an individual.
It is important to select the proper equipment for the person’s needs.
Choosing the wrong product can make the difference between effectively preventing or healing a pressure sore, and not.
Consult with the individual’s doctor or healthcare team to ensure the choice of an appropriate product.
Prevention is Key
Pressure sores can be extremely detrimental to a person’s health, comfort and quality of life, but they can usually be prevented with awareness and precautionary action.
Final Thoughts – Bedsores and Dementia
Older people are more susceptible to bedsores and dementia, especially if they have trouble with mobility. In addition, older people who carry weight, suffer from conditions such as diabetes, incontinence or poor nutrition are at greater risk of developing pressure sores and ulcers.

